Insomnia refers to a chronic or temporary sleep disorder in which a person persistently struggles to fall, stay asleep, or obtain restorative rest. According to a 2024 UK Biobank study published in BMJ Open on insomnia symptom prevalence in England, 29% of adults in the sample reported having insomnia symptoms. The main types include acute, chronic, primary, secondary, onset, maintenance, and comorbid insomnia. Symptoms such as difficulty falling asleep, frequent night waking, and persistent daytime fatigue are characteristic of the condition.
Common causes of insomnia range from psychological stress and anxiety to medical conditions and poor behavioural patterns. Treatments of insomnia encompass cognitive behavioural therapy, sleep hygiene protocols, relaxation techniques, and prescription medications.
Amongst the pharmacological options, diazepam, a benzodiazepine, works for insomnia by enhancing the brain’s GABA activity to induce sedation and reduce sleep onset time. In the United Kingdom, diazepam is a prescription-only controlled medicine, typically obtained through a GP consultation or a Care Quality Commission-regulated online pharmacy.
What is Insomnia?
Insomnia is a clinically recognised sleep disorder characterised by persistent difficulty falling asleep, staying asleep, or obtaining quality rest despite adequate opportunity, leading to significant daytime impairment. According to a 2012 paper titled ‘The natural history of insomnia’ by Jason G. Ellis, national survey data from the USA and the UK show that acute insomnia is highly prevalent, with annual incidence rates between 31.2% and 36.6% depending on how new‑onset versus recurrent episodes are defined.
According to Dr. James O’Donovan, MBBS, PhD, MBA, a Research Director for a global health organisation, Assistant Clinical Professor at Mount Sinai School of Medicine in New York, a Technical Advisor for the World Health Organisation and a licensed NHS doctor, “Insomnia refers to difficulty falling asleep, staying asleep, or waking up too early, despite having the time and environment for rest, and feeling unrefreshed during the day. Now. It’s estimated that 1 in 3 adults worldwide will experience insomnia symptoms at some point in their lives. And around 10% will meet the criteria for an insomnia disorder. Meaning the symptoms are frequent, long-lasting, and disruptive.”
First formally classified as a distinct condition in the 20th century following the advent of clinical sleep research, insomnia works by disrupting the brain’s natural sleep-wake regulatory systems. This results in difficulty falling asleep, difficulty staying asleep, and early morning awakening, all of which produce sleep dissatisfaction, daytime fatigue, and impaired functioning across cognitive, emotional, and occupational domains.
What is the History of Insomnia?
The history of insomnia dates back to some of the earliest recorded civilisations, establishing it as one of the most enduring and universally recognised human afflictions throughout history. Early historical references document sleep disturbances as described in ancient Egyptian, Greek, and Roman texts, where they were often linked to stress, melancholy, or spiritual imbalance. Hippocrates referenced disturbed sleep in his medical writings, whilst Roman scholars attributed chronic wakefulness to emotional excess and constitutional imbalance.
Modern understanding of insomnia evolved considerably with industrialisation, 19th-century medicalisation, and 20th-century clinical sleep research advancements. The invention of the electroencephalogram and the development of polysomnography in the 1950s enabled scientists to study the neurological basis of the different types of insomnia, eventually leading to its formal classification as a distinct chronic condition with identifiable causes, subtypes, and evidence-based treatments.
What are The Types of Insomnia?
The types of insomnias include acute, chronic, primary, secondary, onset, maintenance, and comorbid insomnia, each differing in duration, origin, and characteristic pattern of sleep disruption.
The types of insomnias are listed below.
- Acute Insomnia: Acute insomnia is a short-term sleep disorder lasting from one night to several weeks, typically triggered by a specific stressor, illness, or life event, and presenting with symptoms including difficulty initiating sleep and frequent awakening.
- Chronic Insomnia: Chronic insomnia is a persistent sleep disturbance occurring at least three nights per week for a minimum of three consecutive months, causing sustained impairment to daytime functioning, mood, and cognitive performance.
- Primary Insomnia: Primary insomnia is a standalone sleep disorder not directly attributable to another medical, psychiatric, or environmental condition, arising from inherent dysregulation in the brain’s sleep-wake initiation mechanisms rather than as a secondary consequence.
- Secondary Insomnia: Secondary insomnia is a sleep disorder that occurs as a direct consequence of an underlying condition, such as depression, chronic pain, obstructive sleep apnoea, or substance misuse, and typically requires addressing the root cause alongside the sleep disturbance itself.
- Onset Insomnia: Onset insomnia refers specifically to difficulty initiating sleep at the start of the night, characterised by a prolonged sleep latency period, often associated with psychological hyperarousal, anxiety, or excessive cognitive activity close to bedtime.
- Maintenance Insomnia: Maintenance insomnia is a subtype defined by repeated nocturnal awakening or an inability to return to sleep after waking during the night, often associated with ageing, mood disorders, or pain-related medical conditions disrupting sleep continuity.
- Comorbid Insomnia: Comorbid insomnia is a form of chronic insomnia that coexists alongside another medical or psychiatric condition, such as depression, anxiety, or post-traumatic stress disorder, and requires simultaneous management of both the insomnia and its comorbid condition.
What are The Symptoms of Insomnia?
The symptoms of insomnia include trouble falling asleep, nocturnal awakening, early morning waking, unrefreshing sleep, daytime fatigue, poor concentration, mood disturbances, and compromised work or driving performance.
The symptoms of insomnia are listed below.
- Trouble Falling Asleep: This refers to a persistent inability to initiate sleep within a reasonable timeframe, typically longer than 30 minutes after lying down, which can affect a person’s mood, motivation, and capacity to function effectively the following day.
- Waking Up During the Night: Individuals experience repeated interruptions to their sleep cycle, waking multiple times throughout the night and finding it difficult to return to sleep, significantly reducing total sleep time and the quality of restorative sleep stages.
- Waking Up Too Early: This symptom involves unintended early morning awakening well before the desired rise time, leaving the individual unable to return to sleep and consistently feeling insufficiently rested at the start of the day.
- Feeling Unrefreshed After Sleep: Despite spending adequate time in bed, those with insomnia frequently wake without feeling restored, as the quality and architecture of their sleep is too fragmented or shallow to fulfil the body’s true restorative requirements.
- Daytime Sleepiness and Fatigue: Persistent nighttime disruption results in significant daytime sleepiness, chronically low energy levels, and physical fatigue, all of which can affect a person’s productivity, concentration, and overall capacity for safe daily activity.
- Poor Concentration and Memory Problems: Insomnia directly impairs cognitive performance, manifesting as forgetfulness, difficulty sustaining focus, reduced processing speed, and measurable deficits in both short-term and working memory across academic and professional settings.
- Mood and Emotional Disturbances: Prolonged sleep deprivation is strongly associated with heightened irritability, emotional instability, increased susceptibility to anxiety, persistently low mood, and, in more serious cases, the development or significant worsening of clinical depression.
- Work or Driving Performance Issues: Chronic poor sleep substantially impairs reaction time, decision-making ability, and sustained alertness, creating serious risks in occupational environments and on the road, particularly for those in safety-critical roles or who drive long distances regularly.
How Does Insomnia Affect a Person?
The ways insomnia affects a person are listed below.
- Physical Health Deterioration: Chronic sleep loss weakens immune function and is among the leading causes of heightened cardiovascular risk, obesity, and metabolic dysfunction.
- Mental Health Decline: Insomnia exacerbates anxiety and depression, creating a bidirectional cycle in which poor sleep and compromised mental health mutually reinforce one another.
- Cognitive Impairment: Persistent sleeplessness impairs memory consolidation, attention regulation, and executive function, reducing overall intellectual performance and decision quality.
- Reduced Quality of Life: The cumulative burden of poor sleep erodes relationships, social engagement, and the capacity to sustain enjoyable and fulfilling daily activities.
- Occupational Impairment: Sleep-deprived employees demonstrate lower productivity, higher rates of absenteeism, and substantially elevated risk of workplace accidents caused by errors in judgement.
- Emotional Dysregulation: Insomnia disrupts emotional processing circuits in the prefrontal cortex, making individuals more reactive to stressors and less equipped to manage negative emotional experiences constructively.
What are The Causes of Insomnia?

The causes of Insomnia include genetic predisposition, psychological conditions, lifestyle factors, behavioural patterns, underlying medical conditions, and neurological or biological dysregulation, each contributing distinctly to the onset and perpetuation of sleep disturbance.
The causes of Insomnia are listed below.
- Genetic Causes: Genetic causes of insomnia mean a hereditary susceptibility to insomnia and include variants in circadian clock genes such as CLOCK and PER3. According to a landmark 2019 genome‑wide association study published in Nature Genetics, insomnia shows substantial heritability, with twin and family studies typically estimating genetic contributions in the range of about 25–45%.
- Psychological Causes: Psychological causes of insomnia refer to mental health conditions that overstimulate the central nervous system. The psychological causes include anxiety disorders, clinical depression, post-traumatic stress disorder, and chronic stress, all of which perpetuate cognitive hyperarousal incompatible with normal sleep initiation.
- Lifestyle Causes: Lifestyle causes of insomnia encompass daily habits that undermine sleep quality. This includes irregular sleep-wake schedules, excessive caffeine or alcohol consumption, high-pressure working environments, sedentary behaviour, and failure to maintain appropriate pre-sleep wind-down routines.
- Behavioural Causes: Behavioural causes of insomnia involve learned patterns of maladaptive sleep behaviour. The behavioural causes include associating the bed with wakefulness or anxiety, excessive daytime napping, prolonged screen exposure before bedtime, and chronically inconsistent sleep schedules that fragment circadian entrainment.
- Medical Causes: Medical causes of insomnia refer to physiological health conditions disrupting sleep architecture. This includes chronic pain syndromes, obstructive sleep apnoea, thyroid dysfunction, restless legs syndrome, gastro-oesophageal reflux, and menopause-related hormonal changes affecting sleep continuity.
- Neurological Causes: Neurological causes of insomnia refer to dysfunction in the brain’s sleep regulation pathways. The neurological causes include hormonal imbalances, hyperactivation of the hypothalamic-pituitary-adrenal (HPA) axis, and, in rare cases, fatal familial insomnia, a fatal hereditary prion disease involving progressive, irreversible destruction of the thalamic neurons responsible for sleep generation.
Is Insomnia Life-Threatening?
No, insomnia is not life-threatening directly, but it significantly elevates the risk of serious and potentially fatal health conditions when left untreated over prolonged periods. The indirect risks include an increased risk of heart disease, stroke, type 2 diabetes, and fatal accidents attributable to long-term sleep disruption, impairing physiological homeostasis and cognitive alertness.
According to the research of the American Heart Association, people with insomnia face a 45% higher risk of cardiovascular disease compared with those without sleep disorders. Identifying and addressing these risk factors through timely diagnosis and effective treatment is therefore of considerable clinical importance.
What are the Risk Factors of Insomnia?
The risk factors of insomnia are mentioned below.
- Age: Adults over 60 are disproportionately affected by insomnia due to age-related changes in sleep architecture and increasing comorbidities, making an accurate diagnosis particularly important in this demographic.
- Gender: Women face a higher risk of insomnia than men, largely owing to hormonal fluctuations associated with the menstrual cycle, pregnancy, perimenopause, and post-menopause.
- Psychological Stress: Elevated occupational or personal stress is amongst the most frequent precipitating risk factors, often triggering acute insomnia that can progress to a chronic pattern without timely diagnosis and intervention.
- Pre-existing Mental Health Conditions: Anxiety disorders and clinical depression dramatically increase the likelihood of insomnia onset and often complicate both its diagnosis and its effective management over time.
- Shift Work and Irregular Hours: Occupational schedules that conflict with natural circadian rhythms substantially elevate the risk of developing persistent sleep disorders through chronic circadian misalignment.
- Chronic Physical Illness: Conditions including heart disease, diabetes, chronic pain, and respiratory disease perpetuate ongoing sleep difficulties by directly disrupting physiological comfort and sleep architecture.
How is Insomnia Diagnosed?
The main ways to diagnose insomnia are listed below.
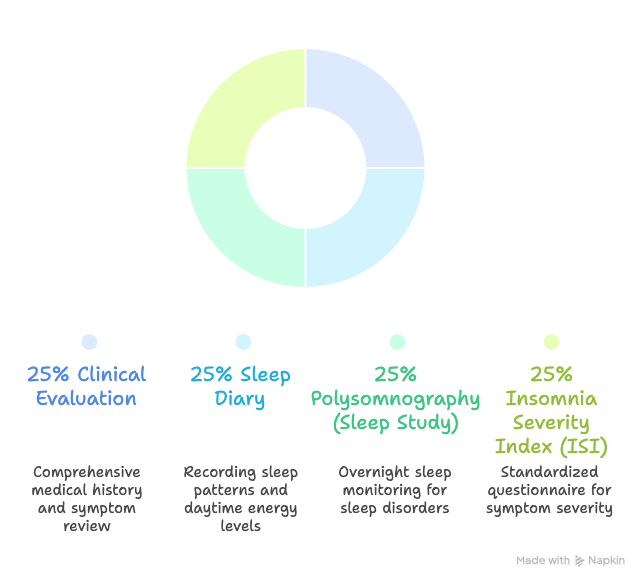
- Clinical Evaluation: A GP or sleep specialist conducts a comprehensive clinical evaluation by reviewing medical history, sleep patterns, lifestyle habits, and daytime symptoms. This is a critical process towards curing insomnia through targeted, individualised treatment planning.
- Sleep Diary: Patients record their sleep and wake times, nocturnal disturbances, and daytime energy levels across one to two weeks, providing objective data to identify patterns and guide clinical decisions.
- Polysomnography (Sleep Study): An overnight polysomnography sleep study monitors brain activity, oxygen saturation, heart rate, and body movement during sleep, primarily used to differentiate insomnia from other sleep disorders such as sleep apnoea.
- Insomnia Severity Index (ISI): A validated, standardised questionnaire that quantifies the nature, severity, and functional impact of insomnia symptoms, widely used in both clinical practice and research settings to track progress and guide treatment.
Can Insomnia Be Cured?
Yes, insomnia is curable or highly treatable via a combination of evidence-based behavioural therapies, lifestyle modifications, and targeted pharmacological intervention where clinically indicated. It can be treated effectively by identifying the underlying causes and making substantive behavioural or lifestyle changes, particularly through cognitive behavioural therapy for insomnia (CBT-I), which is the current NICE-recommended first-line treatment.
Whilst not always a one-time permanent fix, chronic insomnia can be managed and often reversed, leading to normal, restful sleep for the majority of patients who engage with structured treatment.
What are The Treatment Options for Insomnia?
The treatment options for insomnia involve both non-pharmacological and pharmacological approaches, tailored to the type, severity, duration, and underlying causes of sleep disturbance in each patient.
The treatments for insomnia are listed below.
- Cognitive Behavioural Therapy for Insomnia (CBT-I): CBT-I is a structured, evidence-based psychological programme that targets the maladaptive thoughts and behaviours maintaining insomnia through sleep restriction, stimulus control, cognitive restructuring, and relaxation training techniques.
According to NICE guidelines, patients should consult a doctor to access CBT‑I via an appropriate referral, as it is recommended as the first‑line treatment ahead of medication for most adults with insomnia. Clinical studies consistently report remission rates of around 50–60% or higher following completion of a full CBT‑I programme, with sustained improvements maintained at long‑term follow‑up in many randomised trials. - Sleep Hygiene Protocol: Sleep hygiene protocol refers to a set of evidence-informed behavioural guidelines designed to optimise conditions for sleep. This includes maintaining a consistent sleep schedule, limiting caffeine and alcohol, restricting screen use before bed, and creating a cool, dark, quiet sleeping environment.
- Stimulus Control Therapy: Stimulus control therapy is a behavioural intervention that re-establishes the bed and bedroom as conditioned cues exclusively associated with sleep, breaking the learned association between the sleep environment and wakefulness or anxiety.
- Relaxation Training: Relaxation training refers to structured techniques, including progressive muscle relaxation, diaphragmatic breathing, autogenic training, and guided imagery, designed to reduce the physiological and cognitive hyperarousal that impedes sleep onset and maintenance.
- Sleep Restriction Therapy: Sleep restriction therapy is a method that temporarily curtails time spent in bed to closely match the individual’s actual sleep time, thereby building homeostatic sleep pressure that consolidates and progressively improves sleep efficiency through a structured reintroduction protocol.
- Prescription Medications: Prescription medications, including benzodiazepines such as diazepam, Z-drugs such as zopiclone, and low-dose sedating antidepressants, are prescribed by a doctor for the short-term management of severe or treatment-refractory insomnia where non-pharmacological approaches have proved insufficient.
- Melatonin Supplements: Melatonin supplements help regulate the circadian sleep-wake cycle and are particularly beneficial for shift workers, individuals affected by jet lag, and older adults experiencing diminished endogenous melatonin production as part of the ageing process.
Is It Important to Consult a Doctor Before Taking Medication for Insomnia?
Yes, it is important to consult a doctor before taking anti-insomnia medication because self-medication carries significant risks, including dependency, rebound insomnia upon discontinuation, next-day sedation, and dangerous interactions with other prescribed medicines. Medical supervision is required to ensure the correct medication class, therapeutic dose, and appropriate treatment duration are selected based on the individual’s full health profile.
A doctor evaluates and monitors the patient before prescribing by reviewing their complete medical history, ruling out underlying conditions such as obstructive sleep apnoea or clinical depression that may be driving the insomnia, assessing current medications for potential pharmacological interactions, and establishing a structured treatment plan with defined clinical endpoints to minimise the risk of long-term dependence.
What Are the Best Medications for Insomnia?
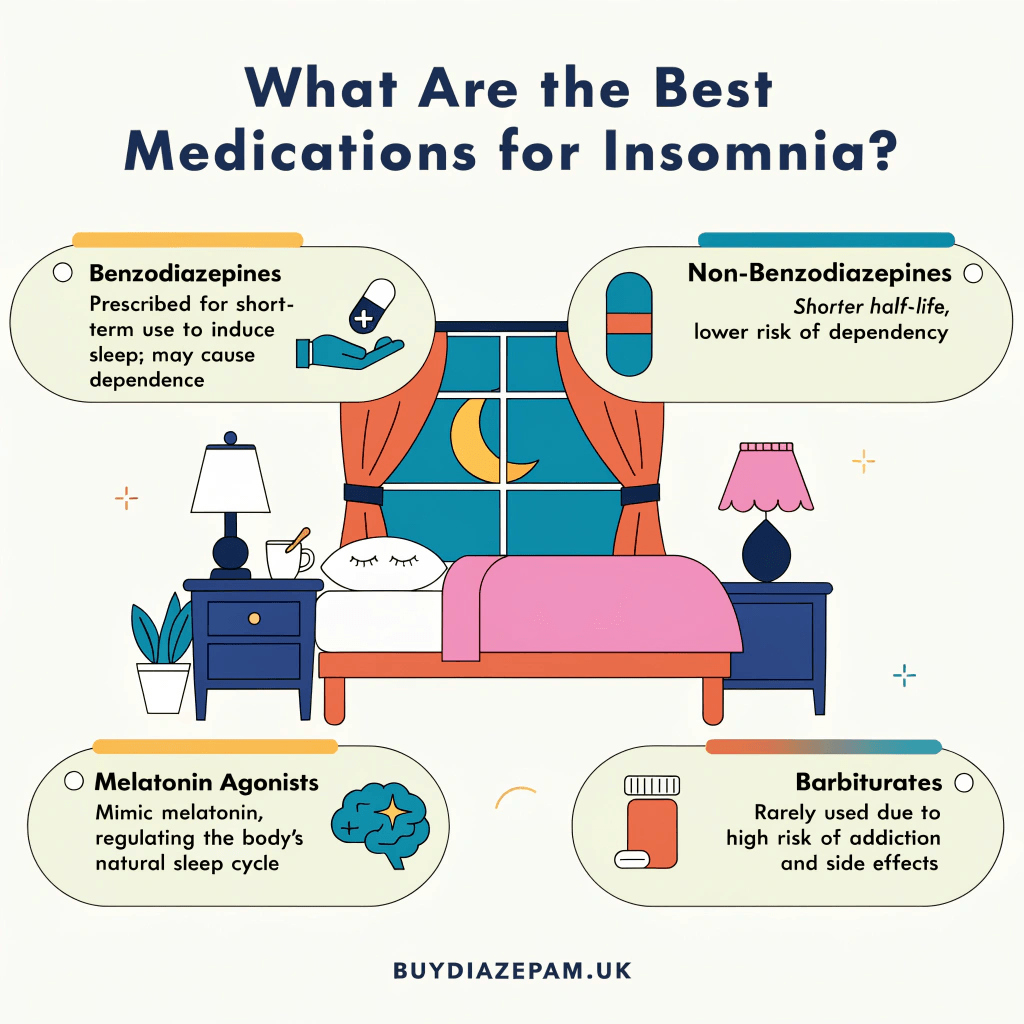
The best medications for insomnia include benzodiazepines, Z-drugs, low-dose sedating antidepressants, melatonin receptor agonists, and antihistamine-based sleep aids, with diazepam being one of the most widely recognised benzodiazepines for short-term insomnia management in clinical practice.
The medications for insomnia are listed below.
- Diazepam: Diazepam is a long-acting benzodiazepine that potentiates GABA inhibitory neurotransmission in the central nervous system, producing sedation, muscle relaxation, and anxiolysis to reduce sleep onset latency and increase total sleep duration.
- Zopiclone: Zopiclone is a Z-drug that acts selectively on GABA-A receptors to facilitate sleep onset and maintenance, prescribed for short-term insomnia management and available exclusively on prescription under UK pharmaceutical regulations.
- Temazepam: Temazepam is a short-acting benzodiazepine indicated for sleep-onset and sleep-maintenance insomnia, prescribed only for brief therapeutic courses due to its high potential for physical dependence and tolerance.
- Melatonin (Circadin): Melatonin (Circadin) is a prolonged-release prescription melatonin formulation licensed in the UK for adults over 55, designed to help re-entrain the circadian sleep-wake cycle with a considerably lower dependency profile than benzodiazepine alternatives.
- Mirtazapine: Mirtazapine is a noradrenergic and specific serotonergic antidepressant with pronounced sedative properties, frequently prescribed at low doses to address insomnia comorbid with depression or anxiety in clinical practice.
- Promethazine: Promethazine is a sedating antihistamine available over the counter in the UK for short-term insomnia relief, though it is not recommended for sustained use owing to the rapid development of pharmacological tolerance.
You can find Valium (diazepam) and other important medicines on our website.
How Does Diazepam Affect Sleep and Insomnia?
Diazepam affects sleep and insomnia by enhancing the activity of gamma-aminobutyric acid (GABA), the brain’s principal inhibitory neurotransmitter, thereby suppressing neuronal excitability throughout the central nervous system and producing pronounced sedation. Diazepam promotes sleep by reducing the time it takes to fall asleep and increasing total sleep duration, making it clinically effective for the short-term management of acute or severe insomnia.
However, diazepam carries significant drawbacks that limit its suitability for long-term use. It reduces deep slow-wave sleep and REM sleep, the most physiologically and cognitively restorative stages of the sleep cycle. So, improper dosing of diazepam can lower overall sleep quality despite increasing total sleep time. Prolonged use is associated with next-day drowsiness, progressive tolerance, physical dependence, and rebound insomnia following cessation, which can be more disruptive than the original sleep disturbance.
Where to Buy Diazepam for Insomnia in the UK Safely?
The common ways to buy Diazepam for insomnia in the United Kingdom safely are listed below.
- NHS GP Prescription: Obtain a valid prescription from a registered NHS General Practitioner following a formal clinical consultation and assessment.
- Private Prescription via High Street Pharmacy: Purchase through a registered pharmacy using a valid private prescription issued by a licensed UK doctor or specialist.
- CQC-Regulated Online Pharmacy: Order from a Care Quality Commission-registered online pharmacy displaying the official EU common logo for verification.
- Private Sleep Clinic: A private sleep medicine specialist may issue a prescription following a thorough clinical evaluation and insomnia assessment.
Can A Person Buy Diazepam for Insomnia Without A Prescription in the UK?

No, a person cannot buy diazepam for insomnia without a prescription in the UK because diazepam is a tightly regulated prescription-only medicine governed by strict controlled drugs legislation. Its legal classification designates diazepam as a Class C, Schedule 4 controlled drug under the Misuse of Drugs Act 1971 and the Misuse of Drugs Regulations 2001, making it unlawful to possess, supply, or purchase without a valid prescription from a registered healthcare professional.
However, in emergencies or special cases, some regulated services, such as Buy Diazepam UK, may facilitate expedited access to diazepam. You can get in touch with us on WhatsApp or Telegram from our homepage to order your desired benzodiazepines.
It is essential to recognise that the various types of insomnia, whether acute, chronic, comorbid, or secondary, present with different symptoms, stem from distinct causes of insomnia, and respond to different treatments and medications. Attempting to self-medicate via buying tracked diazepam or any other meds without professional clinical oversight disregards this complexity. It significantly elevates the risks of misuse, physical dependence, and serious harm to long-term health.


